Meet stroke survivors:
These moving patient stories tell the human side of stroke, and remind us of the experience that over 17 million people worldwide are affected with each year.
Nora's stroke survivor story
Trish's stroke survivor story
Steve's stroke survivor story
Mari's stroke survivor story
Ruth's stroke survivor story
You too can be prepared to help:
Know the warning signs and symptoms for stroke
Many people don’t recognize the signs of a stroke. Knowing them can help you react fast and seek immediate medical attention. Quick action may reduce the effects of a stroke or save someone’s life.
Stroke symptoms depend on the type of stroke (hemorrhagic or ischemic) and the area of the brain that is affected. The length and severity of symptoms can vary drastically from person to person. Although other diseases or conditions may have similar symptoms as stroke, sudden onset is a key factor. The most common symptoms of stroke are:
- Numbness or weakness of the face, arm or leg — often only on one side of the body
- Difficulty speaking
- Difficulty understanding
- Sudden changes in behavior
- Short-term memory loss
- Blurred vision or trouble seeing in one or both eyes
- Dizziness, extreme fatigue, confusion or loss of balance and coordination
- Dilated pupils or sensitivity to light
- Sudden or extremely severe headache, often described as “the worst headache of one’s life”
If you notice any of these symptoms, call your emergency medical service provider and ask the driver to take the person to a certified stroke center in the area. Do NOT attempt to transport the person to the hospital on your own. Hospitals can vary widely in their ability to recognize and provide intervention for acute ischemic stroke.

Understanding stroke
Aneurysm treatment options
Not all aneurysms need to be treated. A treating physician may elect to simply observe the aneurysm over time. However, if an aneurysm is the cause of a hemorrhagic stroke, the treating physician may recommend immediate surgical clipping or endovascular coil embolization. If an aneurysm has not burst (unruptured), but your physician feels that it may be at risk of rupture, he may recommend clipping, coiling or a third option – placement of a flow diverting stent. The treating physician will discuss these options with you and recommend the best course of action based on age, risk factors, size of the aneurysm and your overall health.
The goal of aneurysm treatment is to prevent rupture (in the case of an unruptured aneurysm) or to prevent re-bleeding (in the case of a ruptured aneurysm) by sealing off the aneurysm from the artery out of which it grew.
Endovascular coil embolization
Endovascular coiling is a minimally invasive procedure during which a small incision is made in the groin and small tubes and wires are navigated through the blood vessels to the aneurysm in the brain. Tiny, soft metal coils are then pushed through the tube and placed into the aneurysm. These coils compact to create a tiny metal ball that helps prevent blood flow from entering the aneurysm, thereby relieving the pressure pushing against the walls of the aneurysm.
The Target® Detachable Coil is the world’s leading coil, and is offered in a wide variety of sizes. The treating physician will determine the appropriate size and number of coils needed for a given aneurysm. Due largely to superior clinical outcomes and the elimination of a very invasive procedure with surgical clipping, endovascular coiling has generally replaced surgical clipping as the standard of care for the treatment of many brain aneurysms.
How does an aneurysm coil work?

In aneurysms with large openings from the artery (known as “wide-neck” aneurysms), the treating physician may elect to use additional devices such as a metal stent (a tiny hollow metal tube with holes in it that acts as a scaffold within the vessel) or a balloon.
These devices are designed to help to keep the coils in place inside the aneurysm. In stent-assisted coiling, a permanent stent is placed in the artery where the aneurysm branches off of to help keep the coils in place. Balloon-assisted coiling involves temporarily placing a removable balloon where the aneurysm branches off of the artery in order to help keep the coils in place.
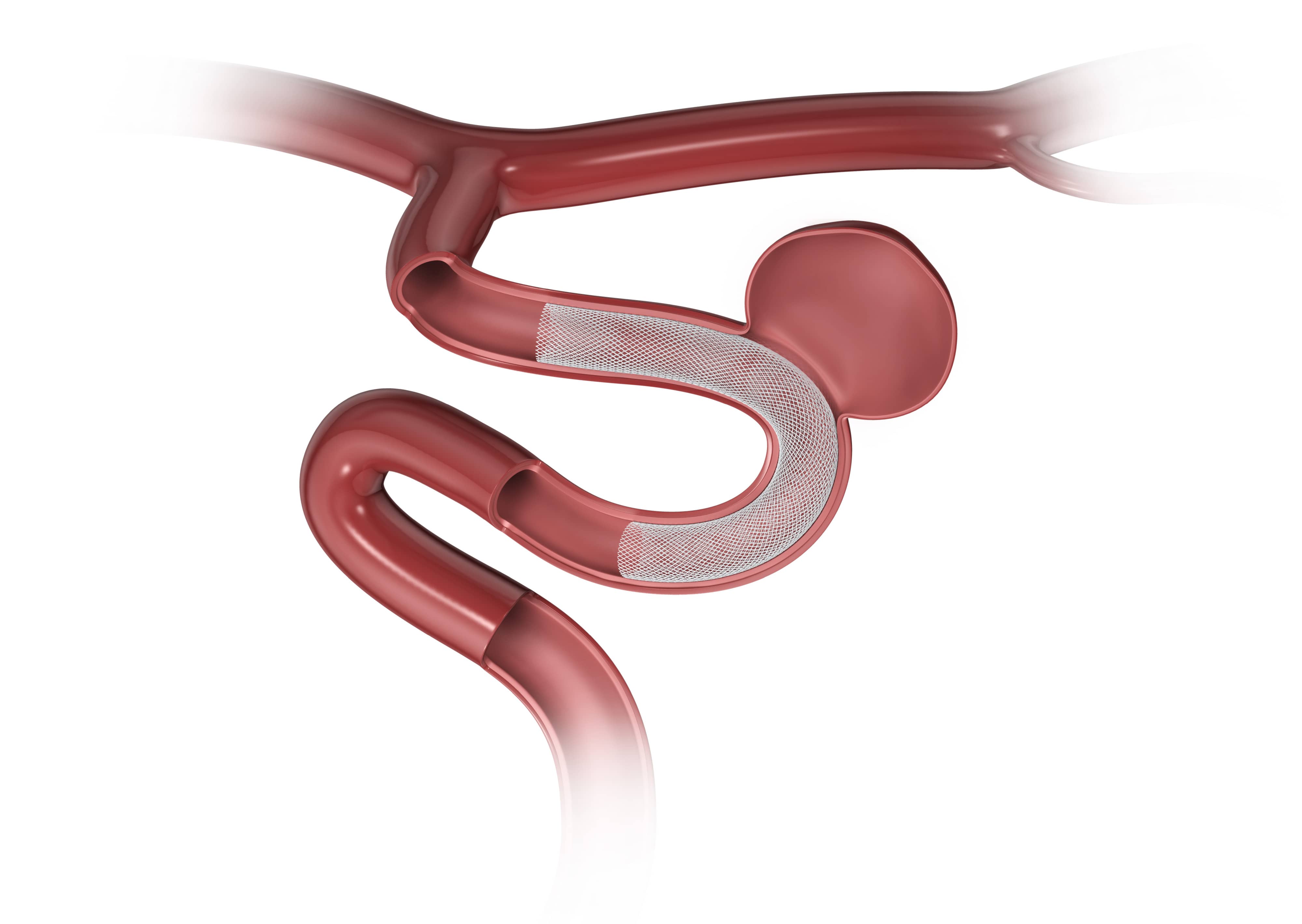
Endovascular flow-diverting stent placement
Endovascular flow-diverting stent placement is a minimally invasive procedure. Typical neurovascular stents that are used in stent-assisted coiling (see Endovascular Coil Embolization) are tiny, hollow metal tubes with holes in them that act as a scaffold within the vessel. Flow-diverting stents are more mesh-like, with much smaller holes. This type of stent is designed to minimize or redirect blood flow away from the aneurysm, potentially reducing the risk of the aneurysm bursting.
Flow-diverting stents are an alternative to coiling for treating unruptured aneurysms. The physician will determine the best course of action based on aneurysm size, aneurysm location, patient age and overall patient health.
Ischemic stroke treatment options
In acute ischemic stroke, the blockage of blood flow is usually caused by a blood clot. The primary goal in treating acute ischemic stroke is to restore the flow of blood to the parts of the brain affected by the stroke by dissolving the clot, removing the clot or by otherwise resolving the blockage. Based on the patient’s symptoms, the blockage location and other diagnostic testing, the treating physician will determine the most appropriate method of care.
Endovascular clot removal
When lytic therapy is not a well-suited option for a patient, the treating physician may recommend endovascular clot removal. There are a number of devices available for removing the clot. The treating physician will determine the best option based on patient anatomy, blockage location and time from symptom onset, among other factors.
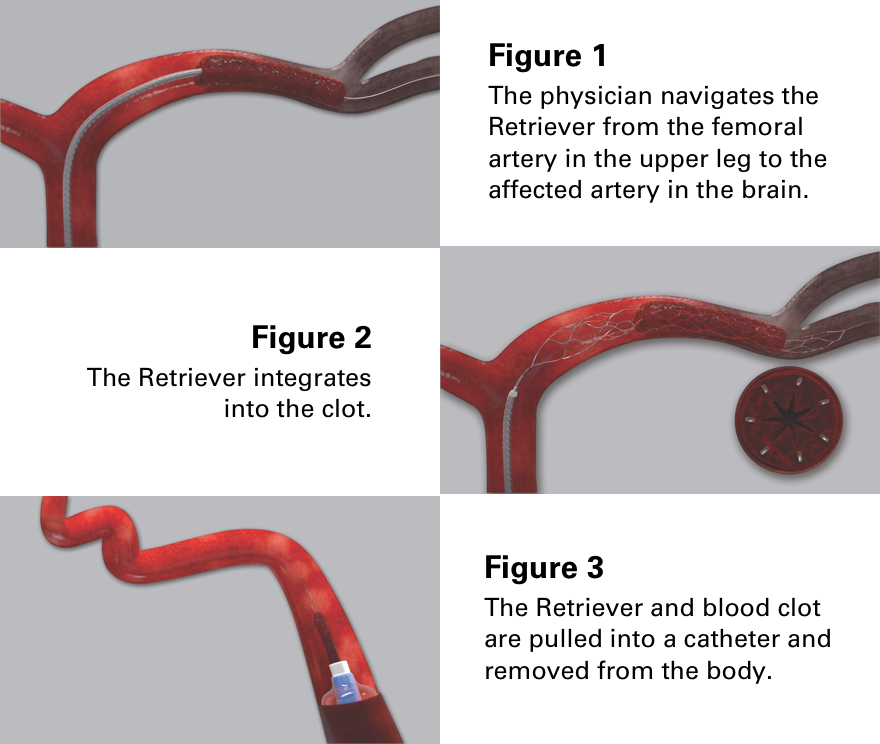
The Trevo® Retriever is a tiny device attached to a thin wire that a trained physician navigates from the femoral artery (located in the upper leg) to the blocked blood vessel in the brain. It is designed to restore blood flow in the brain by removing the blood clot in patients experiencing acute ischemic stroke.
While a growing number of medical centers use the Trevo Retriever to perform the procedure, it is not available at all hospitals.
How does a stent retriever work?